CRT effect on QOL score and NYHA functional class was not influenced by morphology of the BBB (R vs. QRS ≥ 130 ms CRT group: LBBB 87%/RBBB 13% control group: LBBB 86%/RBBB 14%ĬRT improved quality of life, functional status, and exercise capacity in patients with moderate to severe HF, a wide QRS interval, and life-threatening arrhythmias. N = 369 randomized to CRT on (187)/ CRT off (182) followed for 6 months QRS ≥ 120 ms CRT group: LBBB 50%/NSIVCD 32%/RBBB 18% non-CRT group: LBBB 54%/NSIVCD 34%/RBBB 12%ĬRT implant has improved the functional status in all patients that were indicated for ICD and have HFrEF and IVCD.Įxamine the efficacy and safety of combined CRT and ICD therapy in patients with NYHA class III or IV CHF despite appropriate medical management. N = 490 randomized to CRT (245)/control (245) followed for 6 months 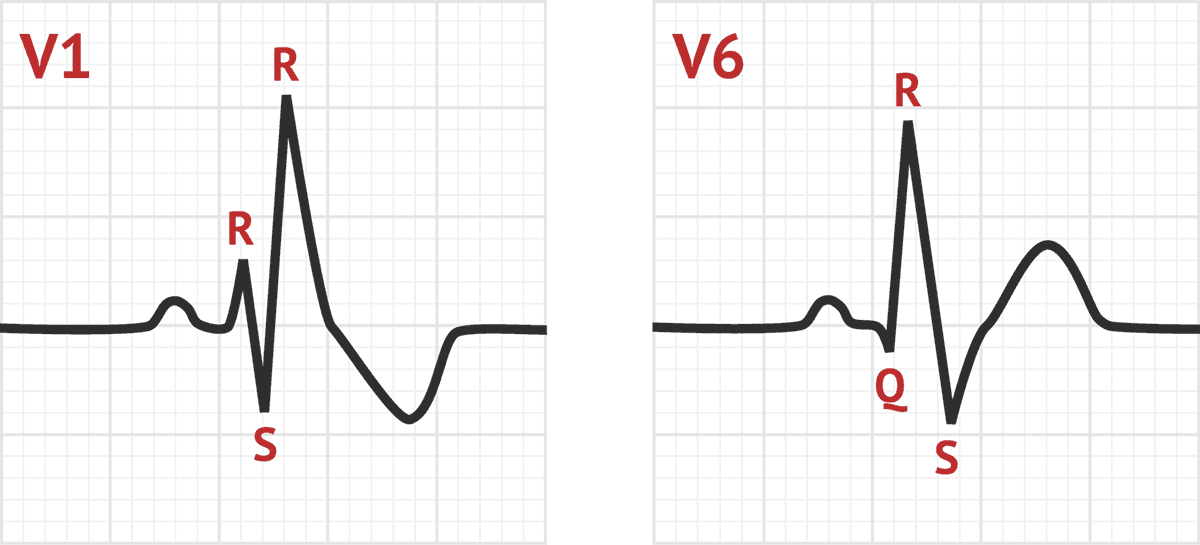
Significant clinical improvement in moderate to severe heart failure with IVCD.Īssess the safety and effectiveness of cardiac CRT when combined with an ICD. N = 453 randomized to CRT group (228)/control (225) followed for 6 months QRS ≥ 120 ms LBBB, 39 (93%)/ RBBB, 3 (7%)ĬRT produces a long-term improvement in the clinical symptoms of patients with HF who have significant IVCD.Įvaluate the clinical benefit of CRT in symptomatic heart failure with IVCD. N = 42 randomized to biventricular CRT (24)/univentricular CRT (17) followed for 9 months Ĭompare the short- and long-term clinical effects of atrial synchronous, pre-excitation of univentricular or biventricular therapy with cardiac CRT. RBBB masks the underlying co-existent LBBB in broader QRS indicating advanced grade of dyssynchrony ( Fig. 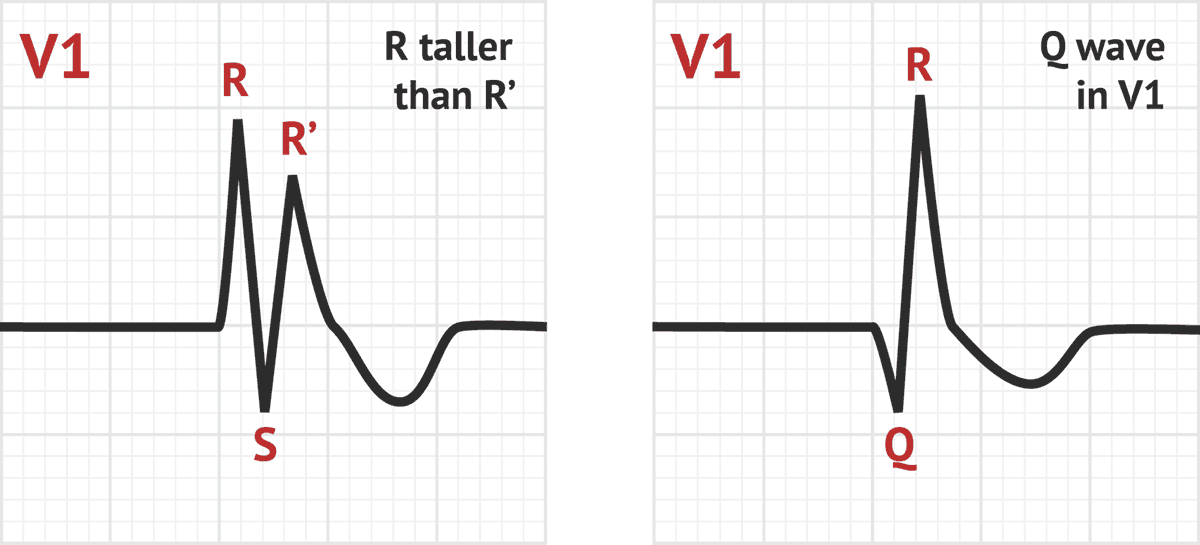
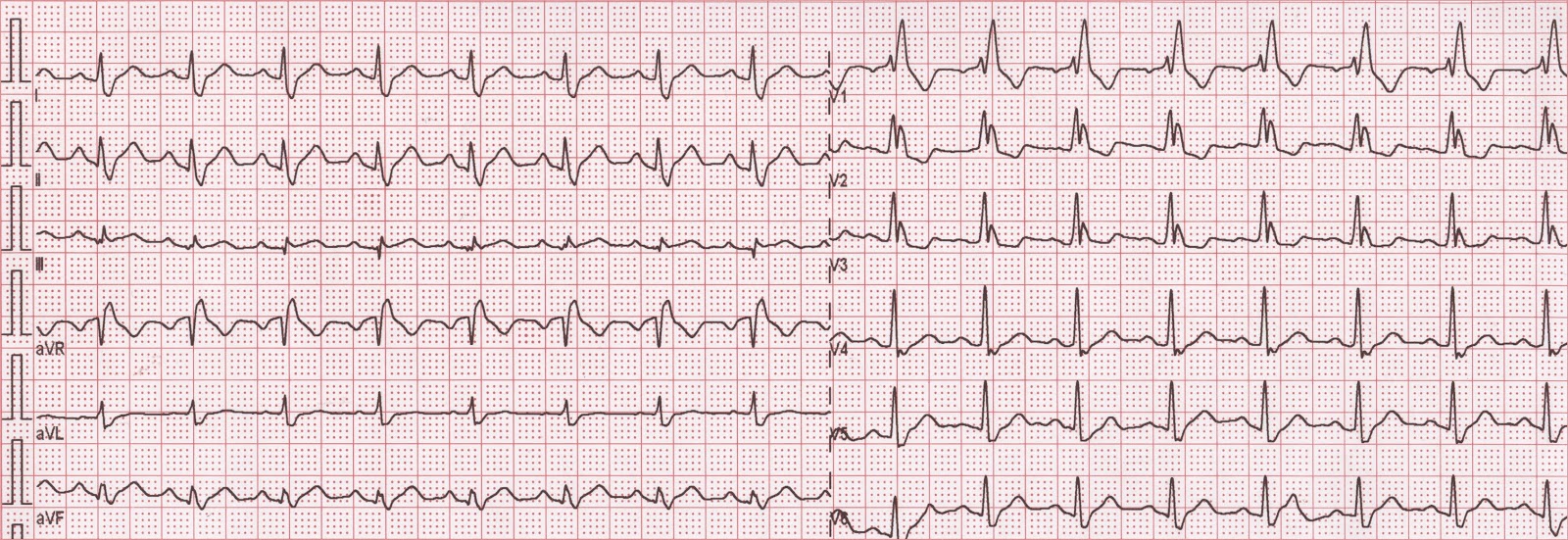
4) Atypical RBBB may represent underlying delay in left ventricular (LV) activation as well. The definition may also be applied to a pattern with RBBB criteria in the precordial leads and LBBB criteria in the limb leads, and vice versa ( Fig. 3) Interventricular conduction delay (IVCD) which characterized by wide QRS morphology that does not resemble either typical LBBB or RBBB. 2) Complete (typical) right bundle branch block (RBBB) is described as QRS duration ≥ 120 ms in adults, rsr′, rsR′, or rSR′ in leads V1 or V2, R or r deflection is usually wider than the initial R wave patients, S wave of greater duration than R wave or greater than 40 ms in leads I and V6 in adults, and normal R peak time in leads V5 and V6 but > 50 ms in lead V ( Fig. Non-LBBB wide QRS complex patterns include the following four groups are represented in Figure 1 as follow: 1) Atypical LBBB represent “QRS duration greater than or equal to 120 ms in adults, broad notched or slurred R wave in leads I, aVL, V5, and V6, and an occasional RS pattern in V5 and V6 attributed to displaced transition of QRS complex, absent q waves in leads I, V5, and V6, and R peak time greater than 60 ms in leads V5 and V6” with atypical feature such as Q wave in I and aVL, larger R wave in V1 and V2, or V6 QRS complex morphology which is different from those in I and aVL ( Fig. The Non-LBBB Wide QRS Complex Electrocardiogram (ECG) Criteria Furthermore, we conferred the current guidelines, including the comprehensive update of the Canadian Cardiovascular Society (CCS) guidelines for the management of heart failure (HF) 2017, the European Society of Cardiology (ESC) Heart Failure Association guidelines for the diagnosis and treatment of acute and chronic HF 2016, the National Institute of Health and Care Excellence (NICE) guidelines for ICD (implantable cardioverter defibrillator) and CRT for arrhythmia and heart failure 2014, the American College of Cardiology Foundation/American Heart Association guideline for the management of heart failure 2013, the ESC European Heart Rhythm Association guidelines on cardiac pacing and cardiac resynchronisation therapy 2013, and the update to National Heart Foundation of Australia and Cardiac Society of Australia and New Zealand guidelines for the prevention, detection and management of chronic HF in Australia 2011. In this article, we reviewed the major trials that enriched the most recent international guidelines for CRT implantation focusing on the available data about the outcome of using CRT in non-LBBB cohort. It remains uncertain whether patients with non-LBBB QRS complex morphology clearly benefit from CRT or only modestly respond. An important and consistent finding in published systematic reviews and in subgroup analyses is that the benefits of CRTs are maximum for patients with a broader QRS durations, typically described as QRS duration > 150 ms, and for patients with a typical left bundle branch block (LBBB) QRS morphology. Cardiac resynchronization therapy (CRT) benefits have been firmly established in patients with heart failure and reduced left ventricular ejection fraction (HFrEF), who remain in New York Heart Association (NYHA) functional classes II and III despite optimal medical therapy, and have a wide QRS complex. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
